The Role of Medicaid Expansion in HPV Vaccine Uptake
HPV vaccination uptake was higher in states that adopted Medicaid expansion than in those that did not, particularly among male adolescents.
Read Time: 2 minutes
Published:
- HPV vaccination rates were higher in Medicaid-expansion states than in non-expansion states.
- The largest gains in vaccine uptake were among Black and Latino male adolescents.
Human papillomavirus, or HPV, is the most common sexually transmitted infection in the United States and is known to cause cancers of the cervix, vagina, vulva, penis, anus, and throat. The multi-dose HPV vaccine can prevent over 90% of cancers caused by HPV and is routinely recommended to all children and youth, aged 9 to 26 years. However, HPV vaccine receipt is relatively low among U.S. teenagers, which suggests families may be facing barriers to vaccination. Obstacles can include infrequent pediatric care, high health care costs, or concerns around vaccine safety.
The Medicaid program in the U.S. has historically helped reduce some barriers to vaccination by covering the full cost of recommended vaccines for all enrolled children. After the passage of the Affordable Care Act’s Medicaid Expansion Program in 2014, states that chose to participate could provide free health care to more than just the lowest-income children. Expansion states now cover a wider group of children and parents, and report higher rates of annual pediatric well-visits than non-expansion states.
Angela Chen and colleagues analyzed data from the National Immunization Survey to determine whether Medicaid expansion affected HPV vaccine uptake among 13 to 17-year-olds. They compared vaccine initiation between states that adopted the Medicaid Expansion Program in 2014 and those that did not.
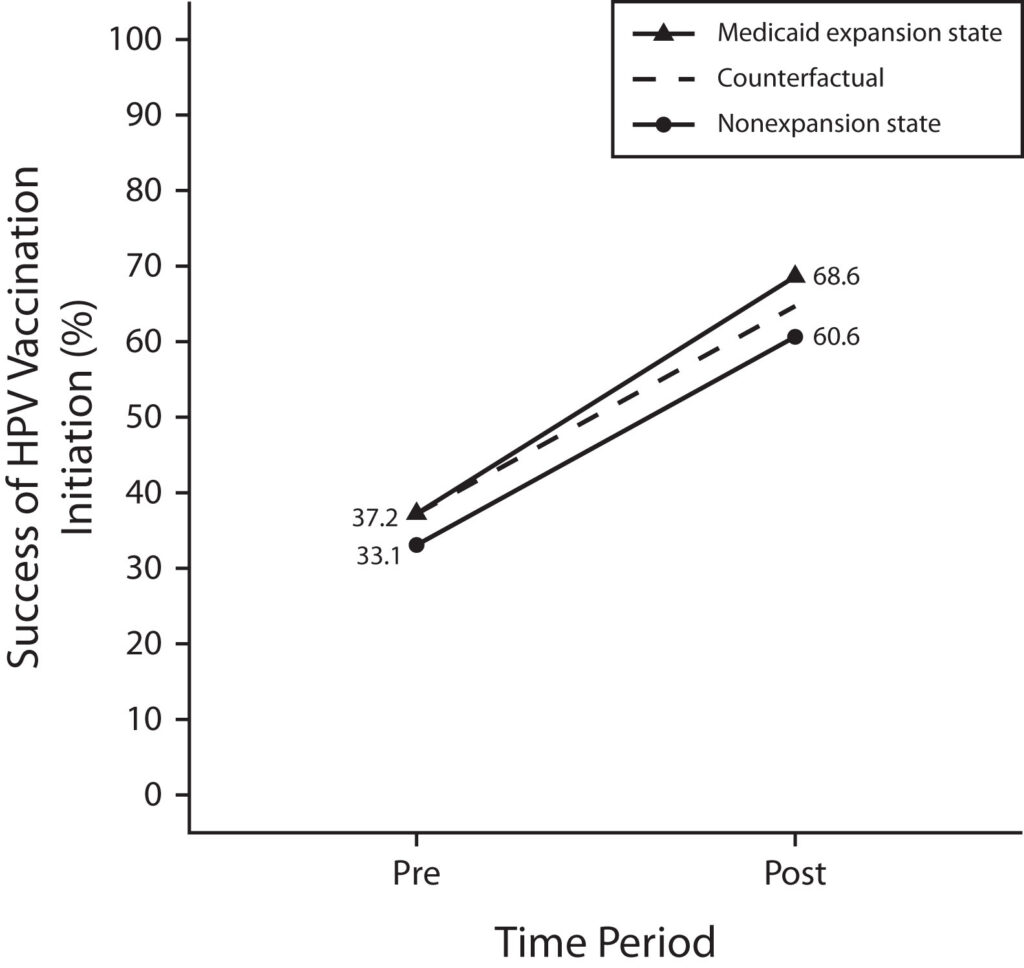
As the figure above shows, HPV vaccine initiation increased in all states from the pre-expansion (2011 to 2014) to the post-expansion (2015 to 2022) period, as males were added to the recommended HPV vaccination population in 2011. Separate from the overall increase, vaccination was substantially higher in states that adopted Medicaid expansion (68.6%) than in states that did not (60.6%).
The largest associations between Medicaid expansion and HPV vaccine initiation were among Black (11% increase) and Latino (13.4% increase) male adolescents, two historically underserved groups in health care. These findings are especially important given that approximately 40% of HPV-caused cancers occur in males.
Chen and colleagues suggest Medicaid expansion may lower certain barriers to HPV vaccination, especially for minority populations. For example, better access to pediatric care in expansion states provides more cost-free opportunities to receive the HPV vaccine and keep up with the multi-dose schedule. Medicaid expansion has also increased the number of parents with health insurance, which may improve parental access to information about the vaccines. The authors argue that Medicaid expansion in all states may be important for achieving optimal HPV vaccination rates across the country.



