Violence is a Public Health Issue
Nearly 20 people are physically abused by an intimate partner in the United States every minute.

Read Time: 4 minutes
Published:

Violence is a Public Health Issue
Nearly 20 people are physically abused by an intimate partner in the United States every minute. One in three women and one in four men are victims of some form of physical violence by an intimate partner at some point in their lifetime. Nearly 18,000 people died from homicide in the US last year, with more than two-thirds of those due to firearms.
Violence is “the intentional use of physical force or power…against oneself or against a group or community…that has a high likelihood of resulting in injury, death, psychological harm.” Globally, nearly 4,000 people die due to violence every day and about 100,000 are injured severely enough that they require medical attention. That is about 36 million people annually, or four times more people than die annually from cancer.
Even as rates of violence from several causes have been declining, the persistent prevalence of violence in our daily lives, both domestically and globally, should give us pause.
In theory, violence is entirely preventable. This should make decreasing violence a top priority in seeking to improve the health of the public—it is fixable. And yet, violence continues to take lives and to injure people worldwide.
Why? There is a rich psychological and sociologic literature about the origins of violence. But we would argue that one reason for the ongoing cost that violence inflicts on us is that we do not think of violence as a health concern. Overwhelmingly we have thought of violence as a criminal justice or social or a political concern. This has resulted in our heavy-handed approach to incarceration that has exacerbated racial divides in the country.
Yet violence is a public health concern, its effects are both individual and collective, and it has a real and present impact on the health of populations. Those who experience violence may die, certainly, but the majority, i.e., those who do not, will go on to experience physical or mental health burdens that can last a lifetime.
It seems worth restating, that violence is an issue of core concern for the health of the public. And solutions to violence must be rooted in an understanding of the context that generates the violence, and of the forces that facilitate it. In no way will this be enough to stanch the costs of violence, but it seems an important first step.
Warmly,
Michael Stein & Sandro Galea

CHIP(PING) AWAY AT COST AND INEQUALITY
An observational study comparing uninsured Medicaid/CHIP-eligible minority children to those who became insured showed large health access and quality gains for the insured group. Children who gained insurance were far more likely to acquire a primary care provider from whom they received both preventive and sick care. Insurance saved $2,886 per insured child per year by reducing hospitalizations and parental work day absences. CHIP’s extension in 2018 could potentially save $8.7–$10.1 billion annually by providing health insurance to all Medicaid/CHIP-eligible uninsured children.
SAVING MONEY AND SAVING LIVES BY TREATING OPIOID USERS
California has the largest number of persons with opioid use disorder in the United States. Yet regulations for publicly-funded treatment facilities in California block access to medication treatment and limit treatment duration—the best hope to avoid overdose. This study, using computer models, shows clearly that offering immediate access to methadone treatment for interested opioid users would have greater health benefits and be less costly ($78,257 per person) than the current standard of care in California. California legislators can change these regulations that limit treatment and use funds from the 21st Century Cures Act of 2016 to address the opioid epidemic while saving taxpayers money almost immediately.

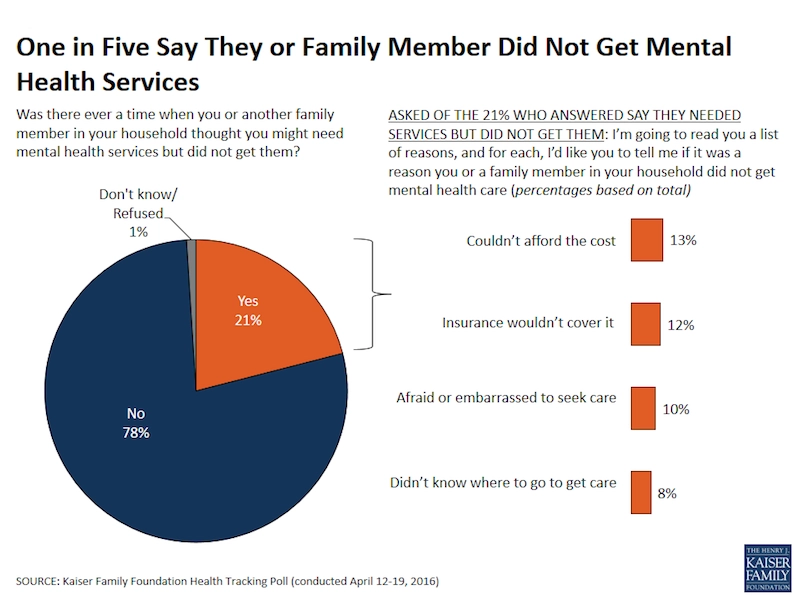
BARRIERS TO MENTAL HEALTH TREATMENT
Data from the Kaiser Health Tracking Poll indicates that millions of Americans skip needed mental health care. The reasons people decided to forgo treatment are instructive. The most common explanation given by respondents had to do with cost and insurance barriers. But almost as many people reported they were too afraid and embarrassed to get help or they didn’t know where to go. These results make it clear that solving the cost problem won’t necessarily increase access to care unless stigma around mental health is removed. —Gilbert Benavidez, PHP Fellow
Kaiser Health Tracking Poll: April 2016, Jamie Firth, Ashley Kirzinger, and Mollyann Brodie.