Children Catching Their Breath
School-based health centers may improve access to health care among low-income, elementary school-age children.
Read Time: 4 minutes
Published:
Pediatric asthma is the most common serious lung disease among children and adolescents in the United States. Childhood asthma leads to preventable outcomes such as hospital stays, missed days at school, and higher health care costs. Rates of asthma and adverse outcomes are higher among non-Hispanic Black children, adding to the long list of troubling health disparities in the U.S.
Policy makers and health care providers increasingly recognize that school-based health centers (SBHCs) can provide important access to primary care for all children as well as asthma care and case management. SBHCs are physically located in or near schools and, at a minimum, provide primary health care and other services (such as dental and mental health care) when possible.
The number of SBHCs in the U.S. grew from 1,135 in 1999 to 2,584 in 2017, reflecting their importance as a medical home for low-income and racial/ethnic minority children. Despite this growth and generally positive effects on children’s health, only 40 % of all SBHCs are in elementary schools and approximately 1,000 of more than 67,000 public elementary schools have an SBHC.
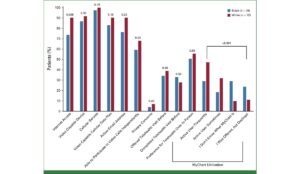
In 2020, our team examined the effects of new elementary SBHCs in three different geographic areas of Georgia (metro, small urban, and rural). These schools also differed with respect to their dominant racial and ethnic student populations: Hispanic (91%), non-Hispanic Black (89%), and non-Hispanic white (91%). This created an opportunity to assess effects on access to primary and preventive care among publicly insured (Medicaid or the Children’s Health Insurance Program-CHIP) children across these areas/groups.
With access to these new SBHCs, well-child visits and flu immunizations increased among children with Medicaid/CHIP insurance in the predominantly non-Hispanic Black and Hispanic schools. Nutrition counseling increased in the Hispanic school. And dental visits increased in the non-Hispanic Black school.
While asthma cannot be cured it can be better managed.
While asthma cannot be cured it can be better managed. In our more recent work, we examined the effects of these SBHCs on asthma case management for children insured by Medicaid/CHIP. Compared to areas without an SBHC, asthmatic children with access to an SBHC were more likely to have 3 or more asthma-related visits and receive asthma-relief. Children in SBHC schools also had greater access to asthma-control medications during the school year. As in our earlier study, we saw these effects only among users of the predominantly non-Hispanic Black and Hispanic SBHCs. These positive outcomes were largest in the SBHC serving mostly non-Hispanic Black students.
These findings point to the potential of SBHCs to improve access to needed health care among low-income, elementary school-age children. A key factor in SBHCs’ success has been the financial sustainability afforded them when Federally Qualified Health Centers (FQHCs) “sponsor” them as their umbrella organization. More than 80% of the current 80 SBHCs in Georgia, along with most other SBHCs nationally, have FQHCs as their umbrella organization.
Although financial sustainability is key to the growth of elementary SBHCs, they can only be effective if families use them as a key point of access to health care for their children. The differences in outcomes seen across the SBHCs we studied indicate that cultural differences and other barriers (language, for example) can reduce their effectiveness. It will be important for the those implementing and managing SBHCs to recognize cultural limitations and barriers across geographic areas (rural versus urban) and racial/ethnic groups (non-Hispanic white versus non-Hispanic Black versus Hispanic) in order to increase community buy-in and use of SBHCs by all eligible children.
We gratefully acknowledge our colleagues and co-authors on the manuscript: Carol J. Hogue, Daniela Franco-Montoya, Peter J. Joski and Jonathan N. Hawley. This work was supported by funding through the National Institute on Minority Health and Health Disparities.
Photo via Getty Images