Broken Justice and the Public's Health
The incarceration rate in the United States (698 per 100,000 people) is higher than any other large country in the world, and nearly five times higher than the median worldwide.

Read Time: 5 minutes
Published:

Broken Justice and the Public’s Health
The incarceration rate in the United States (698 per 100,000 people) is higher than any other large country in the world, and nearly five times higher than the median worldwide. There are about 2 million incarcerated adults, or nearly 1 in 100 Americans. Meanwhile another nearly 5 million people are on probation or parole, for a total of 7 million adults—about 1 in 35 US residents—under correctional supervision.
The chorus of voices showing us how deeply flawed, broken perhaps, our justice system is has grown too loud to ignore. The criminal justice system perpetuates racial inequities in the country that continue centuries of disenfranchisement of minorities. African Americans make up 13 percent of Americans but 40 percent of the incarcerated population. Structural racism, from arrests through sentencing, characterizes the criminal justice system. A for-profit bail bond system means that low-level charges can trap lower income families in a cycle of incarceration that can bankrupt them, destroy families, and deepen class and attendant health divides.
Why does this matter to the public’s health? First of all, jail and prison are profoundly unhealthy environments. Disability-adjusted life years lost linked to incarceration is over double that attributed to other conditions commonly experienced in the general population. Although prisoners are the only US citizens with a constitutional right to health care, they often face delays in access to care, restrictive medication formularies, a lack of acute care options, and understaffing of specialty care medical providers, particularly in the areas of mental health and addiction treatment.
But well beyond this, the health effects of our justice system extend into all reaches of the population. Mother’s incarceration, for example, is associated with a 30 percent increase in infant mortality rate, with a stronger effect among Blacks than Whites. Residents of neighborhoods with high incarceration rates have a two- to threefold increase in rates of depression and anxiety. This likely reflects a combination of the social strain of incarceration among families and a confluence of adverse social circumstances that contributed to incarceration in the first place, compounding the challenges faced by residents of these communities. There is little question that we are consistently underestimating how deeply incarceration influences health.
While a justice system is undoubtedly necessary for social order and safety, a broken justice system compromises the health of the public and deepens the unfairness that characterizes racial health inequities in the country.
Warmly,
Michael Stein & Sandro Galea

DO THE RIGHT THING
Adherence to recommended treatments saves lives after a heart attack, but taking daily medications like aspirin or statins is hard for people to sustain. In a large randomized trial, investigators paid half the participants to take two or more medications (dollar amount based on a daily lottery), sent them reminders, and offered advisors for monitoring, feedback, and reinforcement. The other half received only the usual post-hospital care. Unfortunately, this multi-pronged approach did not increase adherence or improve patients’ vascular health. Even in the aftermath of a serious medical event and when offering incentives, it’s hard to change behavior.
TAKE IT OR LEAVE IT
Nearly two-thirds of bankruptcy is caused by medical costs despite the fact that most costs are paid for by insurers. Some patients will absorb financial hardship to seek medical care, but others won’t, preferring to forgo care, even for serious illness. In this survey, nationally representative participants were asked to value treatments with varying chances of cure and bankruptcy in the presence of a lethal disease. Although the average American values cure more than financial solvency, a cure-at-all-costs option describes the preferences of only a third of the population, and nearly one-tenth of respondents value financial protection over any chances of cure. Patients often face a trade-off between financial and health risk.

WARTS UP?
The human papillomavirus (HPV) vaccine was revolutionary when it hit the market. It was the first vaccination to prevent cancer caused by specific strains of HPV. It also helps prevent anogenital warts, which are growths seen around the anus and genitals. The vast majority of cases are caused by HPV types 6 or 11, both of which are targeted by the HPV vaccine.
A recent study by researchers from the Centers for Disease Control and Prevention used data from health insurance plans between January 2006 and December 2014, including various types of insurance claims, to measure prevalence of anogenital warts in the United States. Information from 35 million individuals was analyzed.
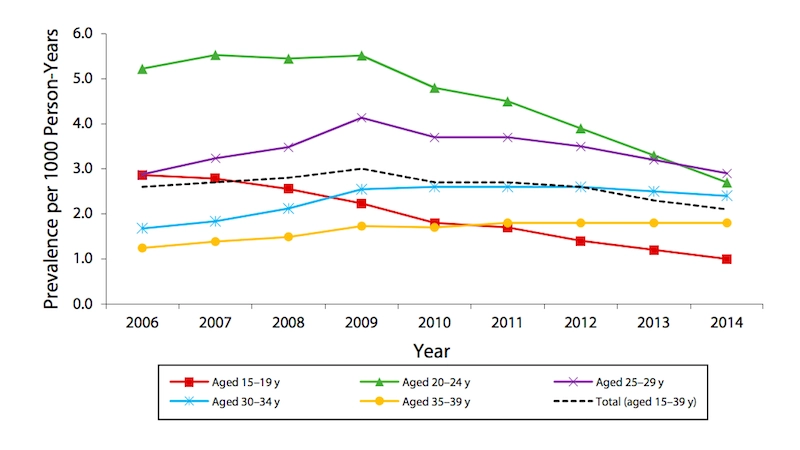
The figure above shows wart prevalence in women. Beginning in 2008 and 2009, prevalence declined significantly in women aged 15 to 19 years, 20 to 24 years, and 25 to 29 years. The decrease in cases was greatest for women between 15 and 24.
The researchers also noticed a significant decrease in anogenital wart prevalence in men aged 20 to 24 years. This is likely not due to men being vaccinated against HPV since vaccination rates in adult men have been low. Rather, the drop is likely due to women being vaccinated and providing herd protection to men who have not been vaccinated. Herd protection refers to population-wide immunity that occurs when a large enough proportion of the population has been vaccinated to slow the spread of disease.
Though herd protection appears to be working to some degree, HPV vaccination rates need to increase. The HPV vaccine is now recommended for women up to 26 years of age and men up to 21 years of age. Nationally, 60% of teens have had one or more doses. Increased vaccination rates among teens and young adults will confer greater protection to the population, further preventing the spread of strains of HPV that lead to both cancer and anogenital warts. —Chrissy Packtor, PHP Fellow
Graph: Elaine W. Flagg, Elizabeth A. Torrone, “Declines in Anogenital Warts Among Age Groups Most Likely to Be Impacted by Human Papillomavirus Vaccination, United States, 2006–2014,” American Journal of Public Health 108, no. 1 (January 1, 2018): pp. 112-119. DOI: 10.2105/AJPH.2017.304119