Healthy Homes

Read Time: 5 minutes
Published:

Healthy Homes
Sixteen million American children live in poverty, putting them at risk for delayed development, disease, and poor educational outcomes. The Earned Income Tax Credit (EITC) is a pro-work, federal tool that has reduced or eliminated poverty for 13.2 million children. Cash transfer programs like EITC improve maternal and infant health.
But 20% of eligible households do not claim this tax credit. More problematically, those families who do seek the refund give away 15-20% of it ($1.75 billion yearly) to for-profit tax preparers.
To lower the U.S. poverty rate which has plateaued, how might health systems help families maximize this economic credit?
Pediatricians are uniquely-positioned, trusted professionals, interacting regularly with low-income families; over 90% of children under two years old see a doctor yearly. A recent program suggests it is possible to connect EITC-eligible families to free tax preparation through physician referral, fliers included with visit reminders, in-clinic advertising, and calls to families with upcoming appointments in the pediatric clinic, offering tax services 15-25 hours weekly, including evenings and weekends. Walk-in visits to a tax preparer, in conjunction with a medical appointment, are available. Families arrive 15 minutes early to complete intake, go to their appointment while taxes are prepared by trained volunteer professionals, and return to finalize their return after the physician visit. Grants, corporate donations, and private philanthropy are used to cover central programming costs (one full-time staff salary, marketing materials, computers).
The program was associated with increased filing rates, receipt of EITC (average $605 refund), and use of free tax preparation, all of which increase money for low-income families. Participants felt more connected to their doctor than persons who didn’t join the program.
Finding such clever, convenient ways to make better use of federal policies to reduce poverty one family at a time creates a novel community resource. Doctors’ offices are one of the only places all families with young children frequent. Targeting predominantly minority, low-income, and Medicaid-insured patients, many of whom are non-English speaking, such tax returns-on-site programs, if disseminated, will permit families to share their financial struggles and enhance the EITC’s underestimated pro-work effect.
For all the talk of the patient-centered “medical home”—a team-based approach for better health outcomes—programs like this one, with a wider view of health creation, are the beginning of a new model: “healthy homes.”
Warmly,
Michael Stein & Sandro Galea

POLICE POLICY
In this era of body cameras, mental health training may improve how police officers respond to situations involving persons with mental health problems. Researchers in England randomized 12 police stations to test the effectiveness of a one-day, professional mental health training for frontline police officers, in contrast to routine training. Police who received this specialized training were better at recognizing mental health issues during incidents in the subsequent six months. The best training design, delivery, and content for training police remains unclear, but this work shows conducting research trials within police settings is feasible and might be acceptable in the United States.
HOW A LEGISLATURE GETS ACTIVE
Changing public policy is one strategy for addressing physical inactivity among children and adolescents. But it is as hard to change policy as it is to get children to exercise 60 minutes a day. This case study describes the development, advocacy for, and passage of Georgia’s SHAPE act, which took six years to unfold and required fitness assessment and physical education for school children to increase their physical activity. Data documenting Georgia’s poor state ranking in childhood obesity were important, but progress was made only after re-framing the legislation as fitness promotion rather than obesity prevention. Bipartisan political support and sponsorships were keys to legislative success here, spurred by diverse community partners, and citizens reached by grassroots outreach and advocacy.

HOME-BASED UPGRADES FOR THE ELDERLY
As people age, day-to-day activities like dressing, bathing, walking up and down the stairs, and managing medications tend to become more difficult and, as a result, more dangerous. Around $219 billion per year is spent on long-term care for those for whom the ability to function independently is impaired.
One alternative to costly assisted living programs or nursing homes is the Community Aging in Place, Advancing Better Living for Elders (CAPABLE) program. CAPABLE aims to help elderly folks with physical disabilities overcome individual or environmental limitations so as to “age in place,” which the U.S. Centers for Disease Control defines as “the ability to live in one’s own home and community safely, independently, and comfortably, regardless of age, income, or ability level.”
As Sarah L. Szanton and her research team found in their study of the effectiveness of the CAPABLE program, health outcomes can improve through home upgrades. In this home-based care model, participants set goals with a registered nurse and an occupational therapist related to independent functioning, and a handyman installs assistive devices, completes home repairs, and increases the safety and overall navigability of homes.
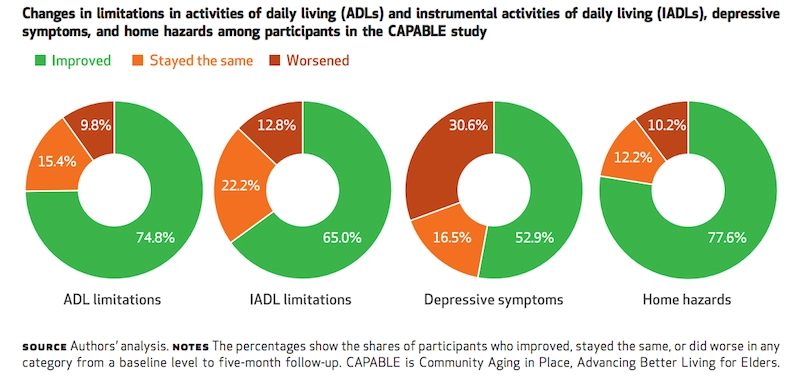
At the end of CAPABLE’s five-month program, 75% of participants were better able to carry out their “activities of daily living” (ADLs). On average, participants were able to halve their difficulties with ADLs, which also reduced symptoms of depression.
Based on these results, the broad use of home-based modifications for those with physical disabilities can save older adults and their families money on housing and health care alongside much-needed improvements in quality of life and mental health. —Madeline Bishop, PHP Fellow
Graphic from Health Affairs Vol. 35, No. 9: “Home-Based Care Program Reduces Disability and Promotes Aging in Place,” Sarah L. Szanton, Bruce Leff, Jennifer L. Wolff, Laken Roberts, Laura N. Gitlin, September, 2016. https://doi.org/10.1377/hlthaff.2016.0140