Environmental Impact Impacts Unevenly
Neighborhood-level environmental factors, like exposure to industrial pollutants, led to increased pediatric ICU admissions for children with asthma.
Read Time: 2 minutes
Published:
The stark racial differences found in several health conditions might arise primarily from differences in social experiences, which then impact health.
This holds true for chronic conditions such as asthma. When compared to White Americans, Black Americans are more likely to have asthma, more likely to go to the hospital for asthma, and more likely to die from asthma.
Recent research examining asthma readmissions in children found that racial disparities could be attributed to a combination of social factors, including socioeconomic status, financial hardship, and the environment.
To further isolate social factors at the neighborhood level that impact severity of pediatric asthma, Jocelyn Grunwell and colleagues compiled data from two children’s hospitals in metropolitan Atlanta and identified patients admitted to pediatric intensive care units (PICU) for life-threatening asthma.
The residential addresses for these patients were mapped according to the 2018 census tracts. Grunwell’s team scored each tract on the Child Opportunity Index 2.0 (COI), which measures the availability of neighborhood resources that encourage child development. This index combines several factors across 3 domains: social and economic, education, and health and environment.
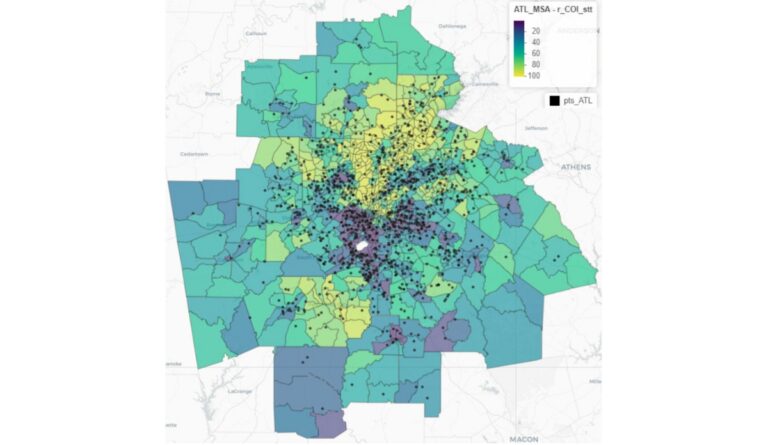
Then the authors percentile-ranked each tract. On the map above, yellow reflects greater opportunity, and purple reflects lower percentiles of opportunity. They noted clusters of PICU admissions and found that these asthma “hot spots” were in areas with lower COI, representing neighborhoods associated with fewer resources.
The authors did explore demographic factors, such as race, but similarly found that neighborhood-level attributes measured by COI’s health and environmental domain (specifically higher exposure to industrial pollutants, airborne microparticles, and ozone concentration) more directly led to pediatric ICU admissions. Their findings highlight the importance of screening for social drivers in pediatric clinical practice when a child struggles with asthma.
Databyte via Jocelyn R. Grunwell, Cydney Opolka, Carrie Mason, and Anne M. Fitzpatrick. Geospatial Analysis of Social Determinants of Health Identifies Neighborhood Hot Spots Associated With Pediatric Intensive Care Use for Life-Threatening Asthma. The Journal of Allergy and Clinical Immunology: In Practice, 2022.



