Denying Climate Change is Denying Health
When we recognize that climate change matters for health, we cannot avoid a discussion of how health is affected in our climate conversations.

Read Time: 6 minutes
Published:

Denying Climate Change is Denying Health
In recent years a few sentinel issues have become third rails in American culture, dividing us along political lines and becoming touchstones for particular parties. One of these issues is global environmental climate change. The current executive branch embodies the Republican party’s general feeling about climate change, espousing a range of positions from the extreme—the earth is not getting warmer—to one of agency—i.e., even if it is, humans have nothing to do with it.
The science on this issue is largely settled. There is little disagreement among scientists that the earth is getting warmer. Hence, the political argument is not really about the science as much as it is about priorities. The Republican party—in the past several decades a ceaselessly pro-market party—values deregulation and corporate interests over the potential negative climate consequences of these same interests.
The question then becomes one of calibrating what we value. If climate change happens slowly and may not affect us for generations to come, how do we make the decision, for example, to limit emissions today?
This is where health may be a useful part of the conversation. We care about health nearly universally. We invest as a country much more on healthcare than any other country. Recognizing that our health is being affected by climate change may give us more data than we can use to determine how much we value the behavioral changes that may be necessary to address climate change with full seriousness.
So, does climate change matter to our health? The World Health Organization estimates that between 2030 and 2050, climate change is expected to cause approximately 250,000 additional deaths per year, from malnutrition, malaria, diarrhea, and heat stress. A paper just released shows that unmitigated climate change will result in up to 40,000 additional suicides across the United States and Mexico by 2050. In the last two decades, as a direct result of climate change, the number of natural disasters doubled from approximately 200 to 400 per year, with human costs rising commensurately. The 2017 hurricane season far exceeded any season in the preceding 30 years. The list goes on.
When we recognize that climate change matters for health, we cannot then avoid a discussion of how health is affected in our climate change conversation. If we are to say—as the current administration is saying—that we do not wish to act on climate change, we are accepting that we are compromising our health. Maybe we are fine with that. We suspect that the vast majority of us are not though, and that if we properly weighted the impact of climate change on our health today and in the years not too far ahead, the national conversation on the issue would be different than it is today.
Warmly,
Michael Stein & Sandro Galea

PUTTING HEALTH CARE IN SCHOOLS
School-based health centers (SBHC) can improve education (high school performance and graduation rates) and health (decreased asthma attacks and emergency room visits generally). In this study of more than 500 public high schools in California, students whose parents didn’t finish 12th grade had lower rates of alcohol bingeing, cigarette smoking, and marijuana use at schools with health centers, although the effects did not extend to Latinos. The convenience, availability, and trust in SBHCs may help address substance use and other mental health issues in high school students. But there may be a differential impact of SBHCs based on student race/ethnicity and socioeconomic status.
CHOOSING FRIENDS WISELY
Substance use usually begins during adolescence, influenced by close friends and social environment. Neighborhoods characterized by high levels of disorder (vacant homes, violent crime, unemployment, poverty) weaken neighborly trust and attachment, produce chronic stress, and undermine adolescents’ sense of control and confidence, increasing risk for marijuana and alcohol use. This study of 13-14 year-olds in Richmond, Virginia who already use at least one substance found that disordered neighborhoods create risks for increasing substance use over time. But this risk is notably reduced by adolescents having a “healthy” peer group, that is, three close friends who have little or no substance use. Healthy peer networks can protect young urban adolescents from harm, although they may be harder to find during the later teenage years.

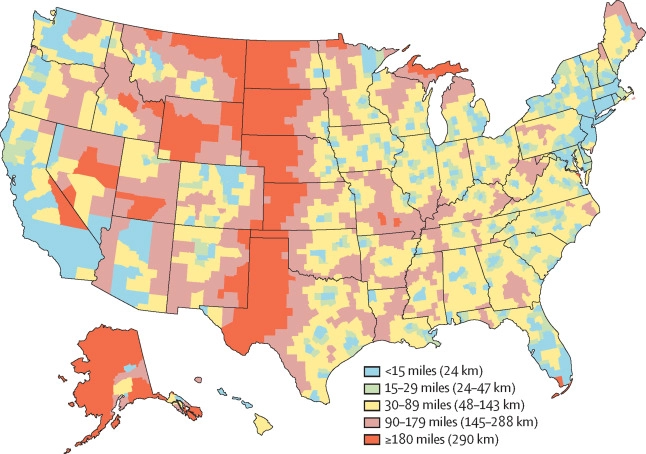
HOW FAR DO WOMEN HAVE TO TRAVEL TO GET AN ABORTION?
Abortion is a common experience for women across the United States. According to the Guttmacher Institute, about one in four women will have an abortion by the age of 45 in the United States. Access to this care can be affected by a variety of factors, including state laws and policies, socioeconomic status, and geography.
As shown in the map above, women who want to have an abortion performed in the middle of the country must travel much farther than women living on the coasts to reach a provider. The red areas indicate that women seeking an abortion must travel 180 miles or more. These areas in the middle of the country tend to be rural, with abortion clinics being concentrated in urban settings. Pink areas can also indicate long travel times that range from 90 minutes to three hours.
The distance needed to travel varies across the country, but it can also vary greatly within a state. In Alaska, about 50% of the women are just over nine miles away from an abortion provider, but 20% must travel over 150 miles to access care. Traveling these long distances can be impossible for women who cannot take time off from work or afford the transportation costs.
Some states that have implemented abortion restrictions in recent years have increased the distance women must travel. In Texas, 20% of women have had their travel distance to the nearest abortion provider increase by about 56 miles. Other states where distance and travel times have increased include Iowa, Montana and Missouri. —Chrissy Packtor, PHP Fellow
Map: Median distance to the nearest abortion provider by county, 2014, Alaska and Hawaii are inset in the bottom-left corner. The Lancet, “Disparities and change over time in distance women would need to travel to have an abortion in the USA: A spatial analysis,” Dr. Jonathan Bearak et al., https://doi.org/10.1016/S2468-2667(17)30158-5




